Mobile health apps improve patient health. Hype or reality?
By Ravisankar CJ on Wed, May 23, 2018
Digital Health has been a hot market space in recent times with investors collectively pouring $26 billion since 2010 and over $7.2 billion just last year. Mobile health or mHealth apps were seen as a crucial element in managing chronic conditions like diabetes and asthma, by helping patients take care of their lifestyle and medications. In fact, mHealth Apps were the largest funded category in digital health, with over 325,000 apps available by end of 2017.
Here is a chart showing the top funded digital health categories since 2010.
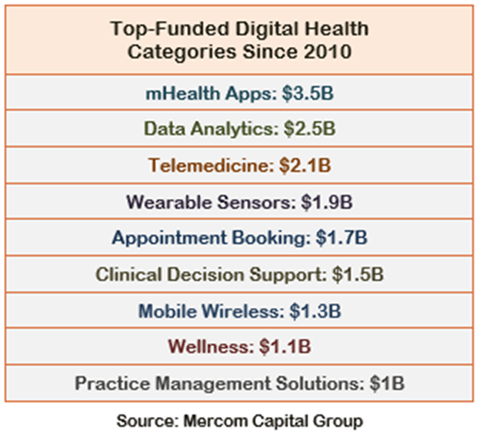
The arrival of mHealth apps has coincided with the change in approach to chronic disease management. From physician-led, periodic clinical visits; it has changed to an integrated approach with continuous monitoring across a patient's daily activities.
These mHealth apps can be of two types. One that helps track a particular disease like hypertension or obesity. Patients can record daily/timely statistics like weight, BP or blood sugar levels that can then be shared with a health care provider.
The other type of mHealth apps is based on patient journey and helps patients with reminders for medication. But do these two type of apps have any effect on keeping the health condition itself under control?
A recently published study looked at exactly this relationship - the impact of medication adherence apps on patients with the condition of hypertension. A sample of over 400 adults with poorly controlled hypertension was taken and a random few were selected to use a smartphone app for medication adherence. The results showed that people who did use the app had a small improvement in adhering to their hypertension medication but had no difference in keeping the blood pressure under control compared to the group which didn’t use the app. So do these mHealth app interventions have any clinical outcomes?
A review of mHealth studies on Clinicaltrials.gov shows only low to moderate impact of mobile app driven interventions. The real solution to impacting patient health is ‘patient-generated data’. To obtain this data - data about their behavior, intention or social factors; patients have to be engaged actively and keep them there. There have to be compelling reasons to use the app and the app has to work on a holistic level – not just one health condition or one process
Data from consumer health technologies, including home-based devices, wearables, and mHealth apps are powering more personalized approaches to patient engagement. Combining patient data with clinical data will help healthcare professionals make appropriate interventions and strengthen this communication loop over time.
The efficiency of these apps can be further improved by building algorithms for automating interventions while using healthcare professionals for other interventions. Take an example of a person with high blood sugar levels. If an app (which takes the daily value of sugar levels from the patient) could automatically organize video visits with certified physicians when the sugar levels go to dangerous levels, it could help keep patients keep their blood sugar levels under control.
There are also other ways in which these apps can engage patients better – taking into consideration related conditions, social factors like income, access to healthy food or behaviors like smoking.
Clearly, people have made the switch to smartphones and there is a large-scale proliferation of apps happening related to health. But the question is, to what extent are apps serving the needs of patients with chronic diseases and their caregivers, as opposed to generally healthy people seeking help with wellness? The answer evidently is - not to a great extent and there
You May Also Like
These Related Stories

How is data playing a part in improving health literacy?

Do Personal Behaviors Drive Better Health Decisions than Doctors?



No Comments Yet
Let us know what you think