Interoperability and Patient Access Rule
Payers now need to publish health information to patients via third-party consumer apps. Payers can also request member’s health history from former payers who had provided services for their current active members. These are the key CMS Interoperability mandate requirements that payers need to comply within July 1, 2021 and Jan 1, 2022.
5 Cents PMPM
Cost to Deploy
100 Days
Days to Deploy
HealFHIR – A managed FHIR infrastructure platform from Sagitec Solutions can help payers to be compliant with the mandate by enabling payers with an infrastructure for provisioning and operationalizing the mandate needs with its following platform capabilities:
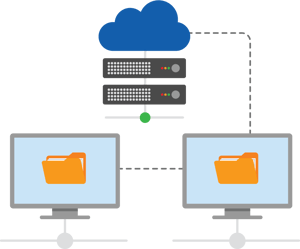
FHIR Infrastructure that is Secured and Hosted in a HITRUST Certified Cloud
Payers will now be able to use their provider and pharmacy network file extracts and leverage HealFHIR converter and loader tools to make them quickly available as FHIR resources to members and consumer apps.
Payers can share adjudicated claim, encounters with capitated provider, and clinical data with patients via FHIR based standard API by leveraging prebuilt HealFHIR claims mapping template and IG conformance validation tools.
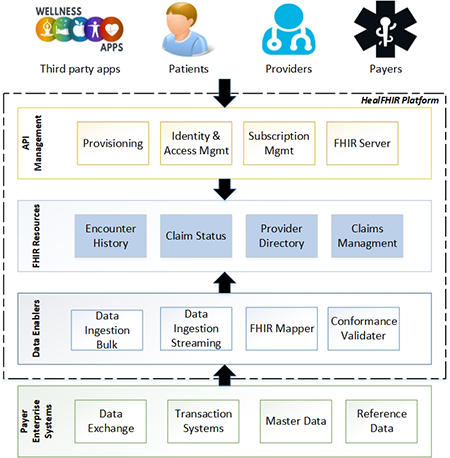
CMS Interoperability Claims Data Mapping and Quality Issues
See What Payers Should Know Before Beginning the Data Mapping Process
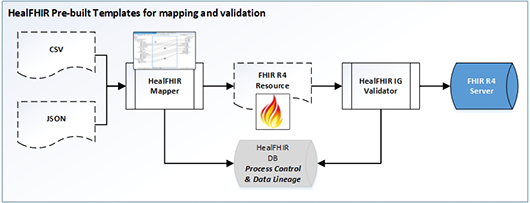
Accelerate the Standardization and Data Movement into FHIR Infrastructure
Sagitec's HealFHIR has prebuilt mapping templates for provider and pharmacy network, claims status, encounter history, and clinical data. This accelerates the mapping exercise to FHIR resources and quickly identify IG conformance gaps. The platform maintains data lineage as the data moves through mapping, validation, and loading phases of the transformation process.
Provision and Manage Access to FHIR Infrastructure
Sagitec's HealFHIR platform comes with the provisioning portal for setting up and managing access to FHIR infrastructure for payers, consumers, and enterprises. This enables payers to define and enforce usage policies for consumers and enterprises while accessing the FHIR infrastructure.
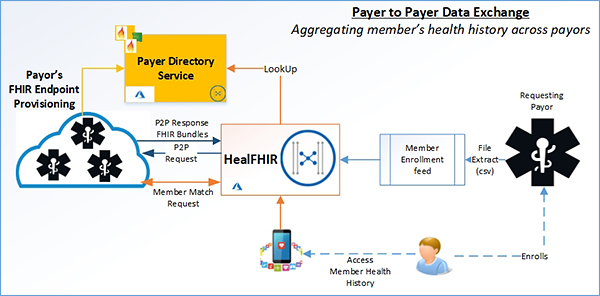
Provide Payer to Payer Data Exchange as a Service
HealFHIR platform takes in a member feed from a payer requesting the health history from the member’s former payer. The solution leverages the payer directory and data aggregation capabilities to fulfill the needs of this data exchange. It aggregates member’s health history data from various payers and provides the requesting payer with an aggregated FHIR bundle. This is a discreate service and does not persist any member data. The managed service will constantly work on provisioning additional payers in its payer directory.
FHIR Compliance Resources
Blog
Resources for Payers
The following are the key focus areas and corresponding enabling resources that payers should be looking for in a vendor solution.
Blog
Cloud Deployment Options
Payers should clearly understand each approach's benefits and drawbacks to help them decide which solution is best for them.
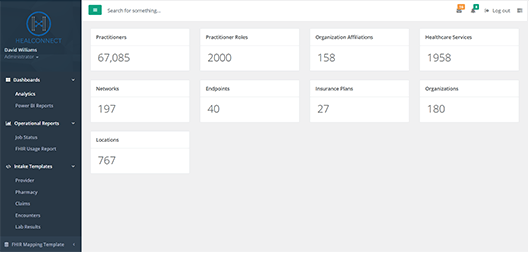
A trial HealFHIR environment is available for payers to quickly upload their provider and pharmacy directory and make them available via FHIR API. The trial environment uses predefined Excel templates to transform and load data into the secured FHIR infrastructure. The HealFHIR dashboard will provide a summarized view of available datasets within the payers' dedicated FHIR infrastructure.
For more information, or to request access to a trial demo, please contact:
Ravi Sankar CJ
Sr. Partner, Sagitec Health
ravisankar.cj@sagitec.com
HL7, FHIR and the [FLAME] mark are the registered trademarks of Health Level Seven International. Use of these trademarks do not constitute an endorsement from HL7.

Provider Directory FAQs
- Should the payer provide real time updates to the provider directory?
- What is the minimum information that the provider directory API should support?
- Should there be a user authentication for accessing the provider directory API?
- Where should the FHIR endpoints be made available?
- Which entities are exempted from this requirement?
Testing for CMS & ONC Conformance FAQs
- Why do we need to test the FHIR infrastructure?
- How would a payer know if the vendor product is conformant to FHIR specification?
- What should be tested?
- What should a payer look for in a vendor’s FHIR conformant report?
- What tools can be used for testing?
Patient Access API FAQs

Founded in 2004, Sagitec has focused on Public Sector and Healthcare industries. Today, Sagitec solutions are used by over 800k+ contributing employers and 5 million+ members. Sagitec’s HealConnect is an enterprise SaaS platform for Medicaid member engagement, deployed on HITRUST certified Microsoft’s Azure cloud.
Contact Us

- 422 County Road D East
Saint Paul, MN 55117

- 612-284-7130
